SPECIAL COVERAGE
Read More
Read More
Judge Denies Trump Motion for Mistrial After Stormy Daniels Testimony
The trial has entered its fourth week, with prosecutors estimating two or three more weeks of trial.
Judge Denies Trump Motion for Mistrial After Stormy Daniels Testimony
The trial has entered its fourth week, with prosecutors estimating two or three more weeks of trial.
Top Premium Reads
Top Stories
Most Read
IRS Asks Tax-Exempt Entities to File Returns Before May 15 Deadline
Entities can seek a six-month filing extension, delaying the due date to Nov. 15.
Biden Condemns Mounting Anti-Semitism in Holocaust Remembrance Speech
‘It’s absolutely despicable and it must stop,’ the president said.
Speaker Says Meeting With Rep. Greene ‘Not a Negotiation’
Rep. Marjorie Taylor Greene made a list of demands that she revealed publicly on May 7.
Sen. Ted Cruz, Rep. Ronny Jackson Push Bill to Help Ranchers Devastated by Texas Wildfires
The Republican lawmakers introduced legislation to expand a federal aid program that assists ranchers whose pregnant livestock are killed in disasters.
Father and Sons Charged for Entering US Capitol on Jan. 6
The FBI received a tip about the family, resulting in the charges.
Trump Says He’s Willing to Go to Jail After Judge’s Contempt of Court Order
‘I have to watch every word I tell you people,’ he told reporters at the court.
Woman Conceived in Gang Rape Says It’s Time to Rethink Abortion Exception
Juda Myers says every person has worth, regardless of the circumstances of their birth.
Republican Contests Dominate Indiana’s May 7 Primaries
High-profile presidential and gubernatorial races have dominated the media, but congressional primaries are likely to generate high interest from voters.
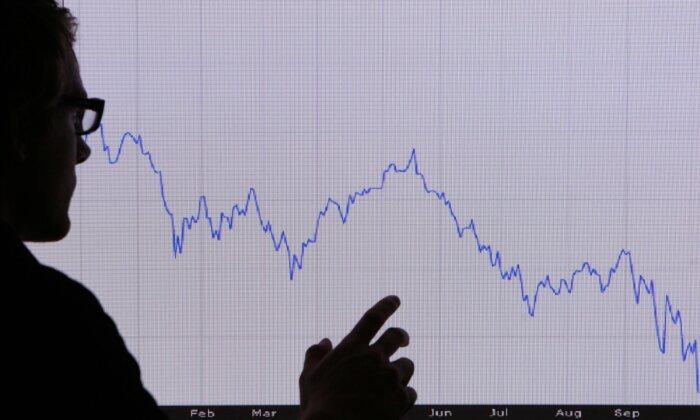
Federal Reserve Will ‘Eventually’ Cut Interest Rates: NY Fed’s John Williams
Patience is vital in bringing inflation back to target.
US Government, Lawmakers Condemn Russia’s Detention of Falun Gong Practitioner
US officials said they are ‘troubled and saddened’ to hear of the Moscow police raid and ‘deeply concerned’ about the persecution of Falun Gong globally.
Social Security Will Go Bankrupt in 2035, One Year Later Than Prior Projections
When the fund goes bankrupt, Social Security benefits will be cut to 83 percent of what they are now.
EU Leaders Confronts Chinese Communist Leader Over Trade at Paris Summit
‘We stand ready to make full use of our trade defense instruments if this is necessary,’ European Commission President Ursula von der Leyen said.
Trump May Seek Sanctions, to Dismiss Charges After Jack Smith Admission
The judge has granted Trump’s request to pause the deadline.

‘Weapons of Mass Migration’: An American Crisis
Director-presenter Josh Philipps points a finger at international organizations helping illegal migration into the United States.
‘Weapons of Mass Migration’: An American Crisis
Director-presenter Josh Philipps points a finger at international organizations helping illegal migration into the United States.
Epoch Readers’ Stories
A History Of The American Nation
A patriotic poem by Ted Schneider
Of Cars and Kids
Why should our kids have to settle for a Trabant, or a Pyonghwa, education when they could have a BMW?
A Nation Divided
Poem by an American Patriot
What Is Going on Here?
There are two major things plants need to survive and continue generating our life saving oxygen. The first is CO2, and the second is sunshine.
Inspired Stories
Empower the World with Your Story: Share Love, Inspiration, and Hope with Millions
Special Coverage
Special Coverage

Birdwatching Improves Student Mental Health: Study
At the end of the experiment, while all groups improved, the birdwatching group ended up with higher scores than both the nature-walk and control groups.

Birdwatching Improves Student Mental Health: Study
At the end of the experiment, while all groups improved, the birdwatching group ended up with higher scores than both the nature-walk and control groups.

From Republic to Dictatorship: The Rise of Sulla
Examining the political feud that led to the near-death of Rome’s Republic.

Stephen Vincent Benet’s Short Story, ‘The Blood of the Martyrs’
This story shows how a meek scientist took a stand for the truth.

‘Tokyo Olympiad’: Japan’s Homage to World Sport
Director Kon Ichikawa gives a beautiful cinematic celebration of our shared humanity.

A Trio of Moon Paintings
The most celebrated painterly moon compositions are three works by the Romantic artist Caspar David Friedrich.

Pythagoras To Beethoven: A Hillsdale College Free Online Music Course
“Join me at the piano,” says concert pianist Hyperion Knight for a free, online course on classical music through Hillsdale College.

Brian Kilmeade’s Love of America and Defense of Its History
The ‘Fox & Friends’ host has written six books that highlight American heroes, establish perspective on U.S. history, and create a sense of gratitude.

A Classical Music Resurgence
Studies over the last two years indicate a rise in popularity of the classical genre and a cultural shift towards more interest in traditional music.

From Republic to Dictatorship: The Rise of Sulla
Examining the political feud that led to the near-death of Rome’s Republic.

Dining Out Woes
Enjoying wine at a restaurant comes with record high prices. Consider dining at home and buying a good wine yourself.

Rick Steves’ Europe: Madrid’s Outdoor Delights
Madrid is best enjoyed on the car-less streets and after the sun sets, when the temperature is more bearable.

Why Adult Children Are Finding Benefits to Traveling With Their Parents
Adult children are giving back to their parents with trips and adventures.

Guatemala Becoming Tourism Hot Spot for Young Travelers
Guatemala is a place to go for adventure but be sure to keep safety in mind.
Rick Steves’ Europe: Madrid’s Outdoor Delights
Madrid is best enjoyed on the car-less streets and after the sun sets, when the temperature is more bearable.






















![[PREMIERING MAY 9, 8:30PM ET] Weapons of Mass Migration | NEW Documentary](/_next/image?url=https%3A%2F%2Fimg.theepochtimes.com%2Fassets%2Fuploads%2F2024%2F04%2F30%2Fid5640415-1920x1080-no-epochtv.jpg&w=1200&q=75)

![[PREMIERING MAY 9, 8:30PM ET] Weapons of Mass Migration | NEW Documentary](/_next/image?url=https%3A%2F%2Fimg.theepochtimes.com%2Fassets%2Fuploads%2F2024%2F04%2F30%2Fid5640415-1920x1080-no-epochtv-1080x720.jpg&w=1200&q=75)
































![[PREMIERING MAY 9, 8:30PM ET] Weapons of Mass Migration | NEW Documentary](/_next/image?url=https%3A%2F%2Fimg.theepochtimes.com%2Fassets%2Fuploads%2F2024%2F05%2F04%2Fid5643663-900x1350-600x900.jpg&w=1200&q=75)

















































































![[PREMIERING 5/7, 9PM ET] The Giant UN Agency Hijacked by Hamas: Asaf Romirowsky](/_next/image?url=https%3A%2F%2Fimg.theepochtimes.com%2Fassets%2Fuploads%2F2024%2F04%2F07%2Fid5645334-240501-ATL_Asaf-Romirowsky_HD_TN-600x338.jpg&w=1200&q=75)