Your health is a deeply personal affair. Your habits, health care access, and family history all play a significant role.
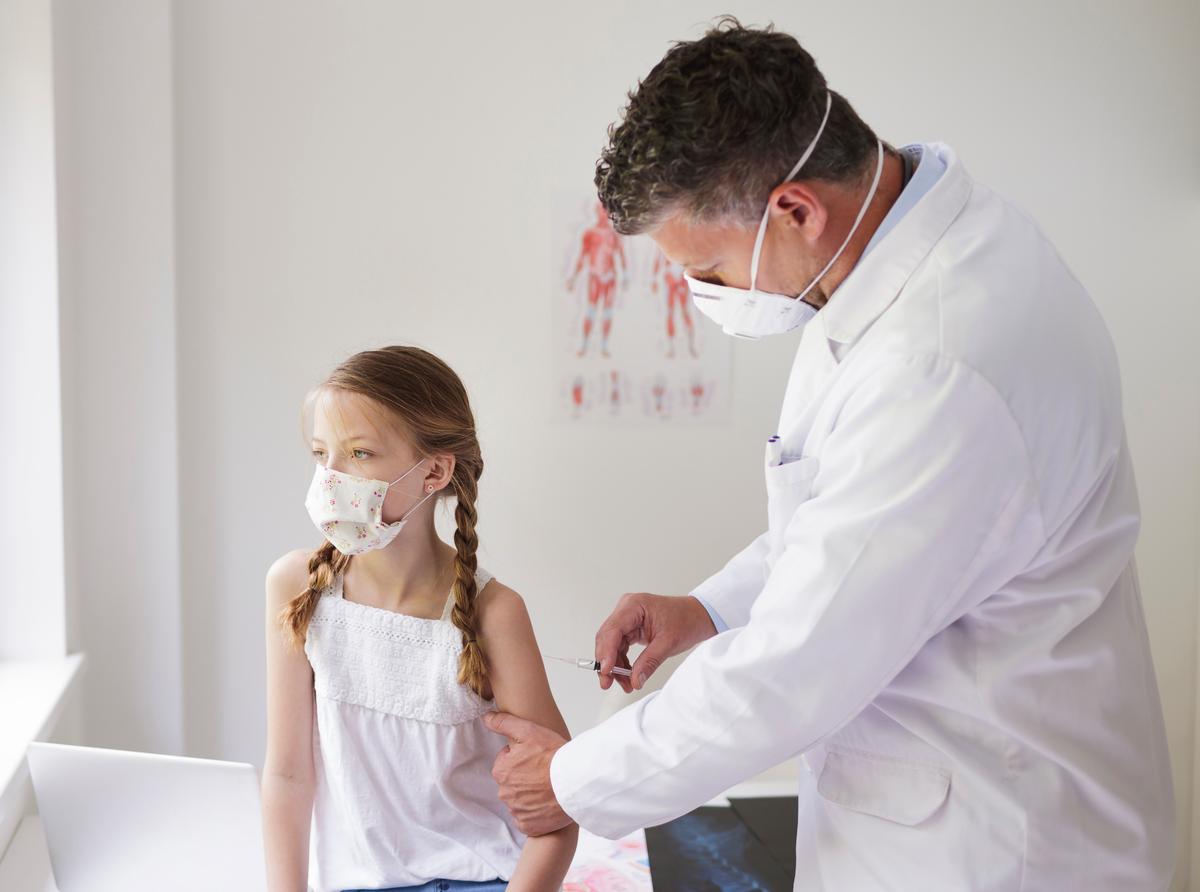
However, one place where health care is generally uniform is vaccines. For now, we have a choice as to whether to take the new COVID-19 vaccine. Meanwhile, all states have a list of vaccinations for several diseases that are mandatory once children enter public school. Although most states allow parents to waive this requirement for religious or medical reasons, opting out is strongly discouraged.