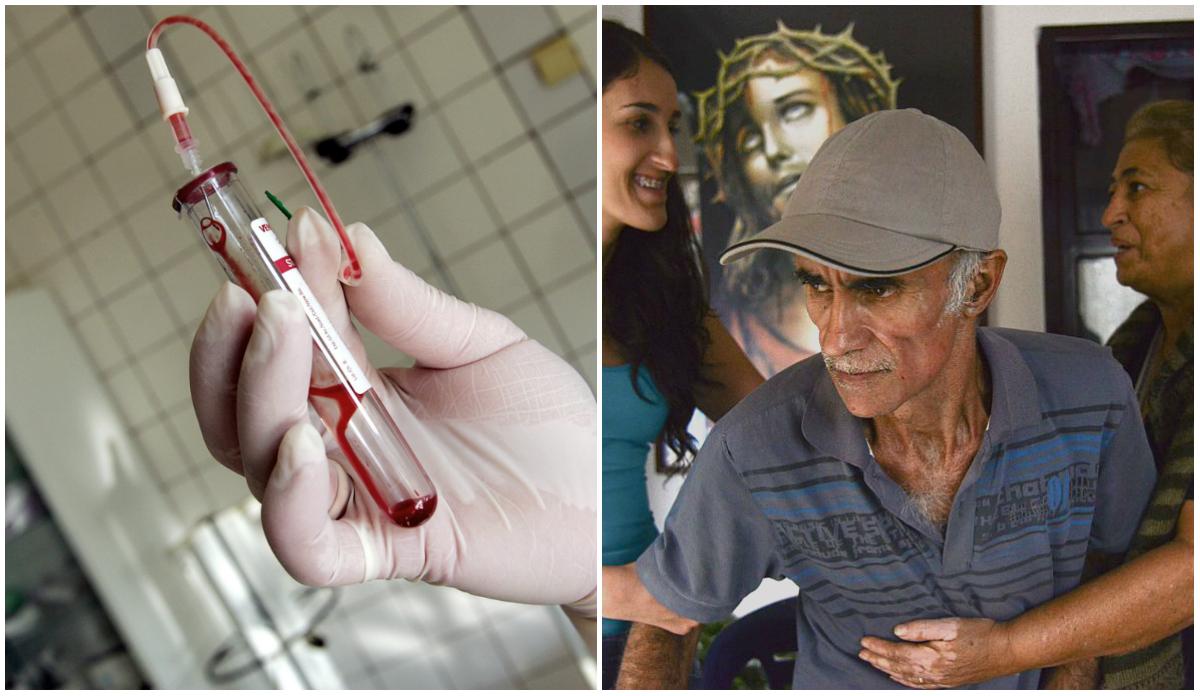
Researchers say a new test could potentially detect Alzheimer’s disease in patients many years before any symptoms arise, sidestepping complicated detection procedures with a simple blood test.
Scientists have long known that a certain protein marker is produced in the body as brain cells die. Current procedures to detect the biomarker involve tapping the spine to access cerebrospinal fluid, which is invasive and expensive.