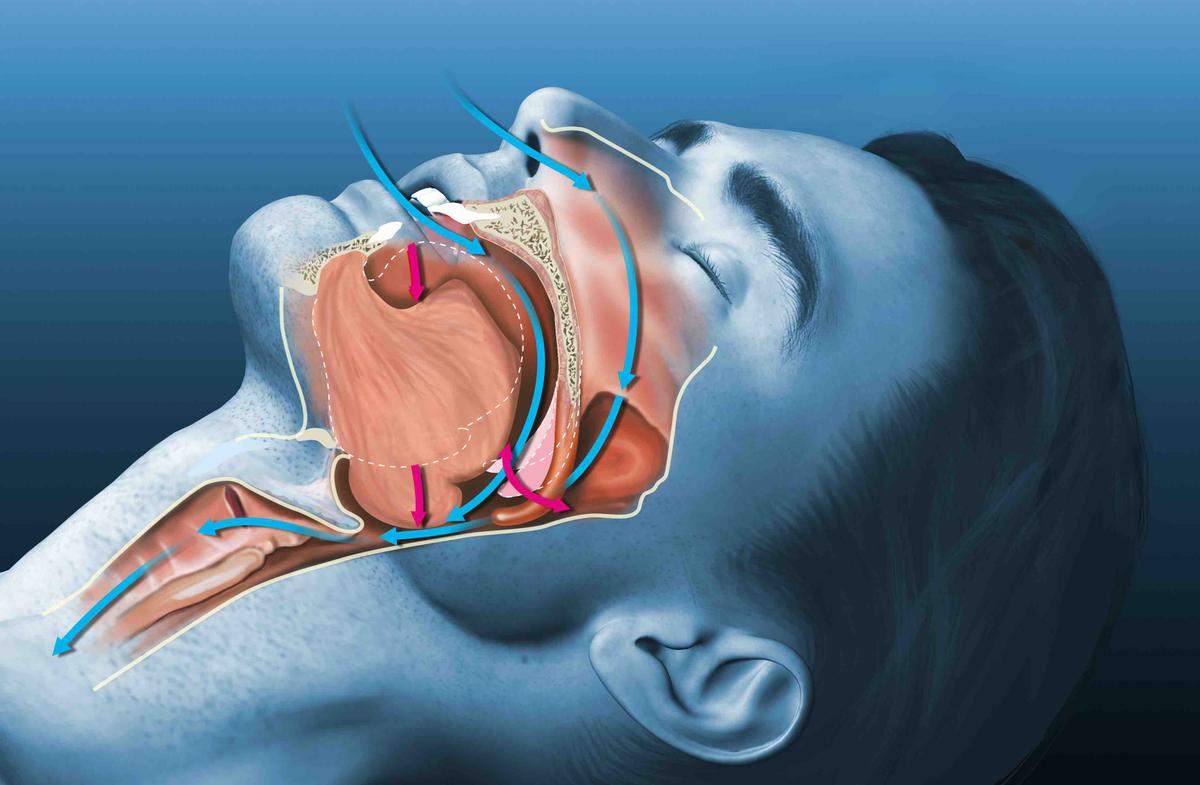
Sleep apnea is a common condition in which your breathing stops and restarts many times while you sleep. This can prevent your body from getting enough oxygen. You may want to talk to your healthcare provider about sleep apnea if someone tells you that you snore or gasp during sleep, or if you experience other symptoms of poor-quality sleep, such as excessive daytime sleepiness.
There are two types of sleep apnea.
- Obstructive sleep apnea happens when your upper airway becomes blocked many times while you sleep, reducing or completely stopping airflow. This is the most common type of sleep apnea. Anything that could narrow your airway such as obesity, large tonsils, or changes in your levels can increase your risk for obstructive sleep apnea.
- Central sleep apnea happens when your brain does not send the signals needed to breathe. Health conditions that affect how your brain controls your airway and chest muscles can cause central sleep apnea.