Medical intuition is a common concept held among many doctors and healthcare professionals–it occurs when a sort of gut feeling or intuitive understanding about a patient’s ailments are “sensed,” even when there are no physical findings.
It has played a critical role in times of emergency and in life-threatening cases. In some cases, hunches have also led to the discovery of medical treatments.
Seven modern real-life cases are illustrated below.
1. A Strange Solution Just in Time
The following story was told on the website of the Center for Spirituality and Healing at the University of Minnesota: “Watching her patient bleed to death on the operating table, heart specialist Dr. Mimi Guernari spent hours trying everything she knew to stem the flow. Then, ‘out of the blue I thought of something I’d never used before and haven’t used since: gel foam.' This intuitive answer made her blink and wonder if she was hallucinating as she watched the bleeding stop. It saved her patient’s life.”
2. An Unexpected Connection
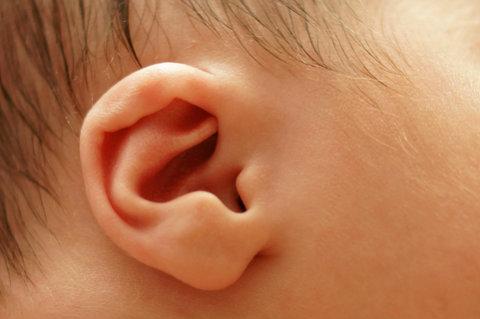
Image of a baby’s right ear via Shutterstock
The following story was told in an article published by the Seattle Children’s Hospital Research Foundation: Dr. Daniel Rubens, an anesthesiologist, wanted to seek an answer to the unsolved riddle of Sudden Infant Death Syndrome (SIDS). He listened to his intuition and sought to examine the relationship between inner ear problems and SIDS. He consulted various professionals who had statistical data on children. He discovered that a hearing deficiency in the right ear often existed in children who had SIDS, which was consistently lower when compared to babies who had not died from SIDS.
3. All Seemed Well, But Thankfully This Nurse Followed Her Intuition

A file photo of a motorcycle after an accident. (Thinkstock)
A nurse tells her story of intuition, quoted in a graduate thesis titled “See Everything, Hear What Is Not Being Said: A Phenomenological Investigation of Intuition in Novice Registered Nursing Practice,” by Lisa A. Ruth-Sahd at The Pennsylvania State University:
“A 44-year-old man came to the hospital after being involved in a motorcycle accident in which he was thrown off of his bike into the guardrail and slid approximately 40 feet. This occurred as he had attempted to avoid hitting the car in front of him that had come to a complete stop. I was surprised that he was alert and oriented on arrival to the emergency department and was able to recall the events of the accident because when the accident occurred he was not wearing a helmet. When he arrived he had stable vital signs …
“Despite these normal findings, I felt apprehensive and uncomfortable and could not understand why. I had taken care of many trauma patients before who were much more unstable than this man, yet for some reason this situation felt different. I kept second-guessing my assessment and wondering why I continued to feel that something is wrong. I looked around the room at my colleagues; no one else seemed to be concerned, as the trauma resuscitation efforts were progressing just like it would for any patient. Although I had just completed an assessment ten minutes earlier with benign results, I felt I needed to go back in the room and perform a second complete assessment.






