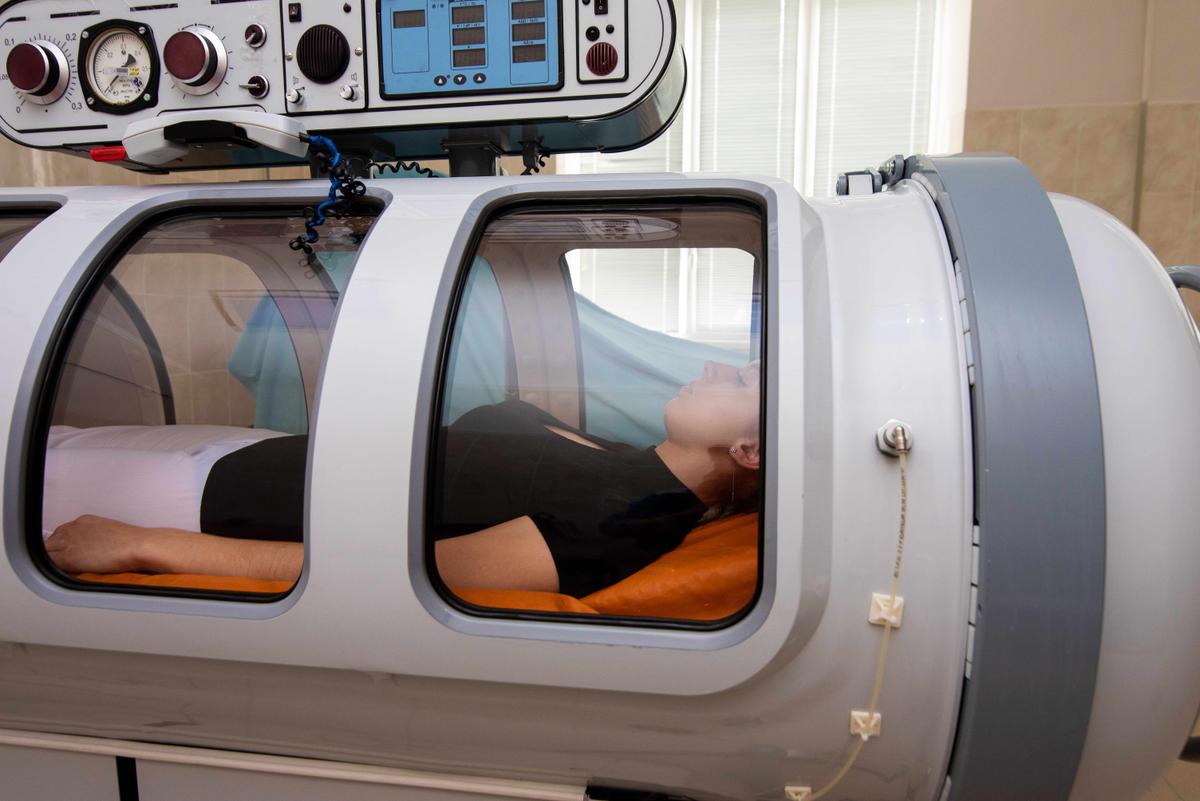
Do you ever feel like you need to breathe deeper than you’ve ever breathed before? Modern life’s daily stressors can deplete your body and make you feel lifeless, but hyperbaric oxygen therapy may help.
GreenMedInfo is dedicated to investigating the most important health and environmental issues of the day. Special emphasis will be placed on environmental health. Our focused and deep research will explore the many ways in which the present condition of the human body directly reflects the true state of the ambient environment. This work is reproduced and distributed with the permission of GreenMedInfo LLC. Sign up for their newsletter at https://greenmedinfo.com/newsletter
Author’s Selected Articles