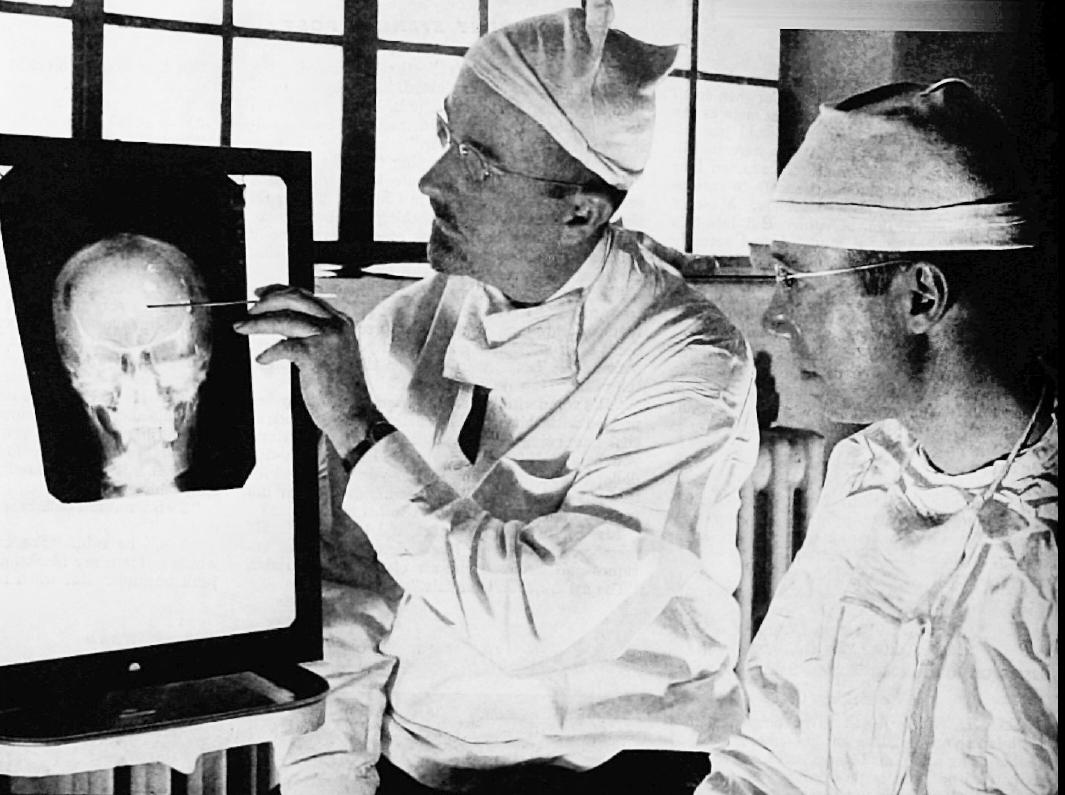
PT is a 78-year-old man who developed debilitating essential tremors in which his arms and hands would constantly shake. It got to the point where he couldn’t write his own name or even hold a cup of coffee. His neurologist tried different medications but they had little effect—other than giving him serious side effects.
His neurologist was a sharp and well-studied physician who referred him to a neurosurgeon to perform deep brain stimulation surgery (DBS). DBS involves the delivery of electrical stimulation to deep brain structures via implanted electrodes connected to an implanted generator (in the chest). Electrodes are run from this generator into the area of the brain that initiates the tremors, which are then connected to a power pack. There is a wireless receiver that can control the amount of stimulation and alleviate most if not all of the shaking.