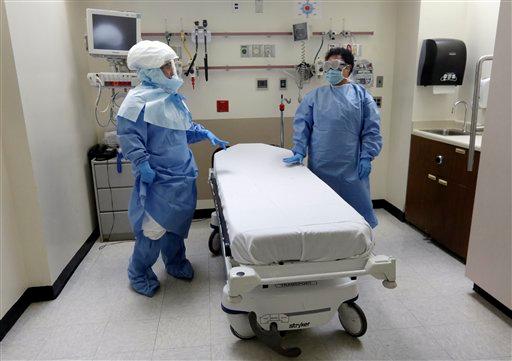
An epidemic disease such as Ebola brings suffering to more than those who get ill or die. Social and economic threats can actually outstrip the medical ones. The outbreaks of SARS in 2003, for example, cost the world economy some US$40 billion, partly as a result of highly disputed travel bans.
Epidemic diseases nearly always also lead to stigmatisation and ill treatment of groups associated with the disease. And because there are always people who are especially scared, epidemic diseases can cause social disruption by people who do such things as flee cities, swamp doctors and health services while well, and stockpile food or medicines.
We can’t entirely eliminate these costs, but we can minimise “Ebolanoia” by addressing fears and directing people to positive actions. Here are some of the risk communication lessons our health officials and political leaders should be mindful of when they engage with the public about Ebola:
1. Don’t Panic About Panic
Governments and health officials think their job is to stop people panicking. They do this by telling people not to panic and by making emphatic pronouncements that the risk of community transmission is very low or that we are well prepared. But they over-reassure. We say “over-reassure” because this tactic does not eliminate fear and it disastrously erodes trust if it fails to address the complex reality that underlies simple statements, or worse, if it is later proven to be wrong.
Telling people not to panic can ironically strengthen the conceptual link between Ebola and panic – a bit like asking people to think of any colour but red.
Worse, it belittles genuine concerns. Australians who worry about Ebola do so because they see a brutal scenario unfolding in West Africa and they can imagine it happening here. The seemingly relentless physical disintegration that the virus causes in the human body inspires dread. The absence or failure of normal mechanisms of control such as vaccines, treatment drugs and in-patient infection control amplify that fear.