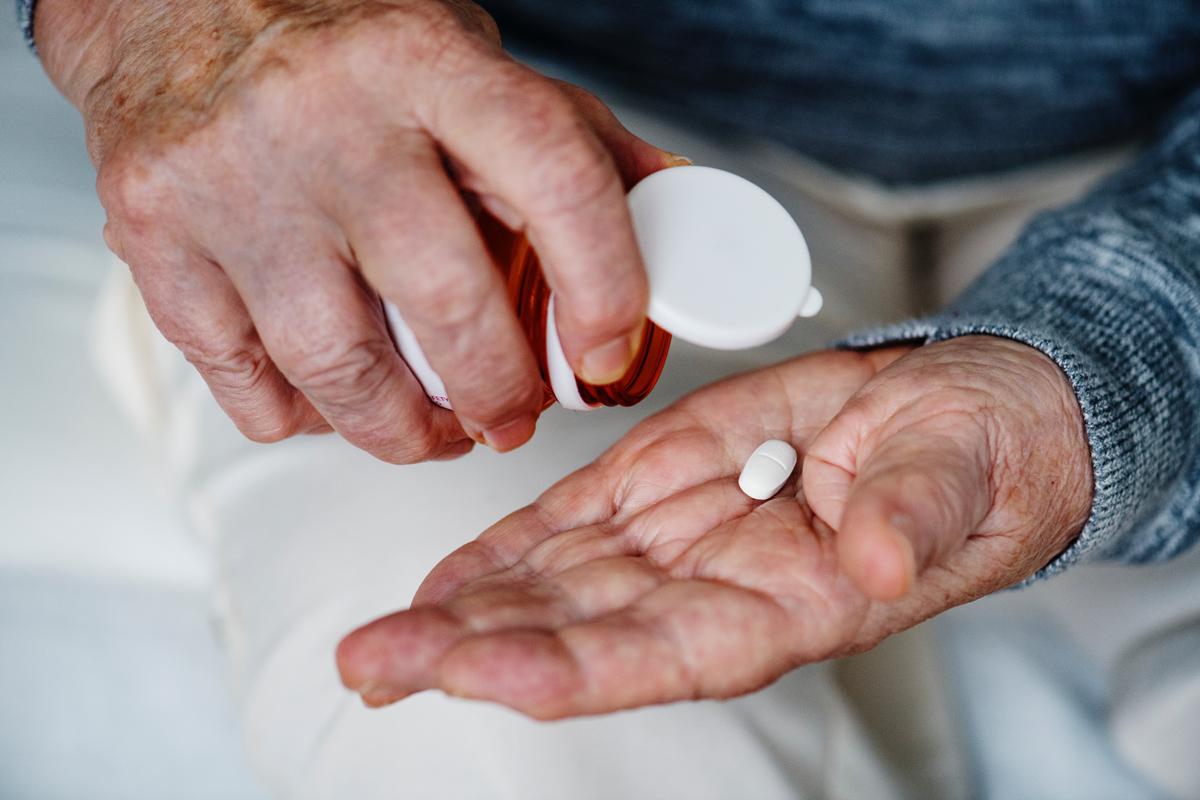
Many surgeons write prescriptions for opioid pain medications four times larger than what their patients will actually use after common operations, according to new research.
And the size of that prescription may be the biggest determining factor in how many pills they actually take, outweighing pain scores, the intensity of the operation, and personal factors, the study suggests.