The well-known actor Michael J. Fox was diagnosed with Parkinson’s disease at the age of 29. At the time, he was one of the most famous celebrities in show business. He gradually developed symptoms such as tremors, stiffness in the limbs and difficulty speaking, and later became a great advocate for awareness and research of this disease. Parkinson’s disease is better treated if detected early, and there is a way to self-test and prevent it.
The Earliest Sign of Parkinson’s Disease
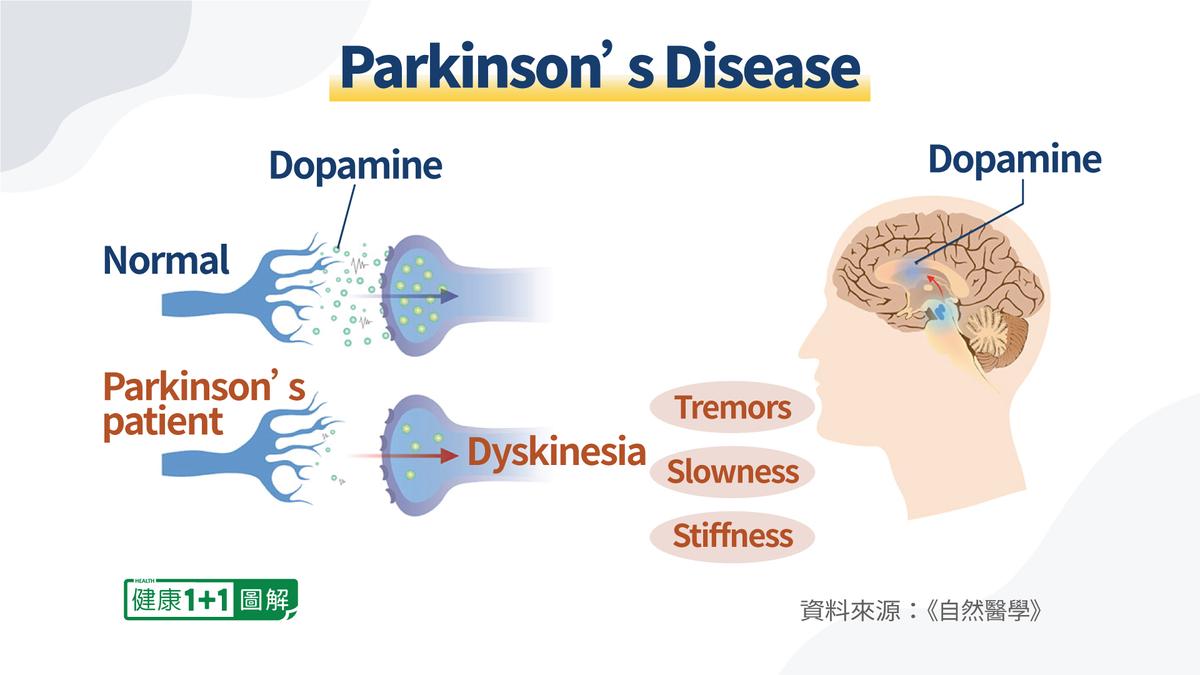
It is well known that Parkinson’s disease can cause dyskinesia, that is, uncontrolled and involuntary movements like twitches.In fact, Parkinson’s disease has another early symptom. That is, most people with Parkinson’s disease have problems with their sense of smell five to 10 years before the onset of the disease’s obvious symptoms such as stiffness in the limbs.