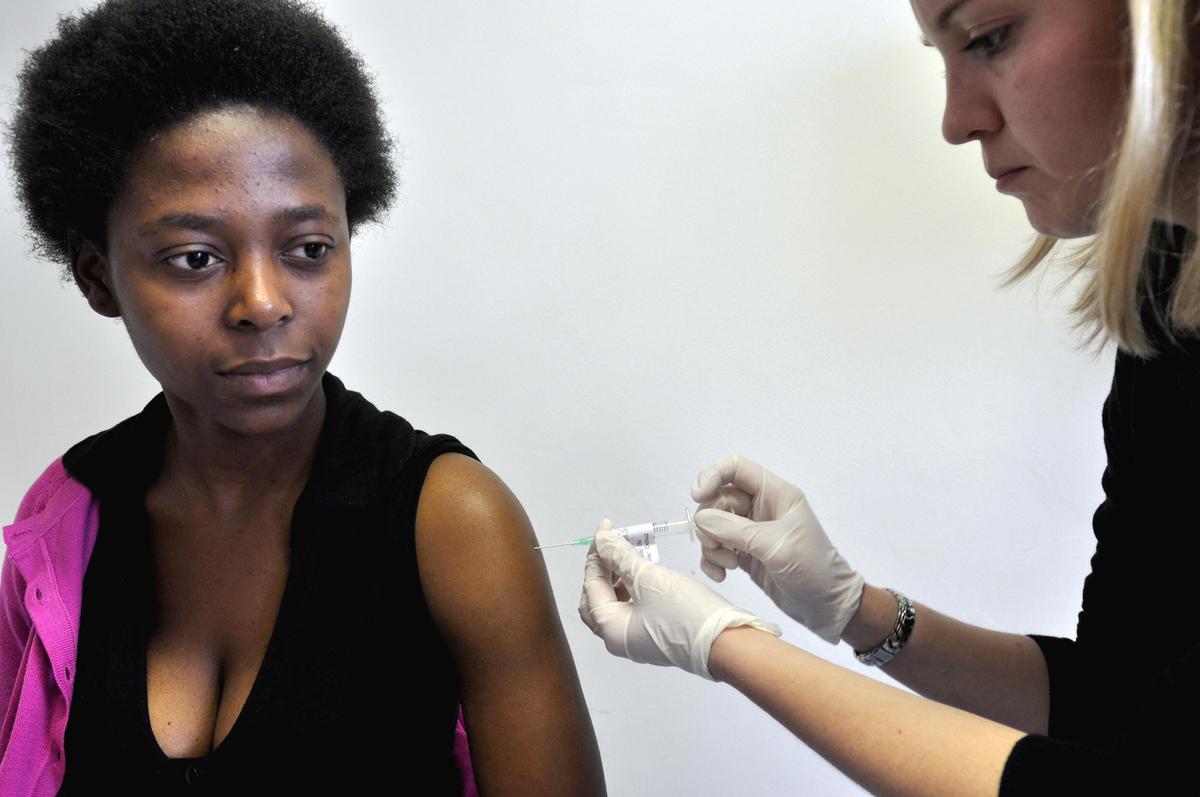
There is no doubt that the crisis caused by the HIV pandemic requires urgent and bold steps. While the roll-out of anti-retroviral therapy has had a significant impact on the epidemic, there are still 1.5 million deaths and 2 million new HIV infections globally every year. In South Africa alone, there are over 6 million people living with HIV. Only 42 percent of these people are being treated with anti-retrovirals.
In the long-term, the use of anti-retrovirals to control the HIV epidemic is unrealistic. Our best hope for an AIDS-free future is the development of a vaccine. Two major clinical trials are set to begin in South Africa in 2016. Both seek to test whether antibodies, which circulate in blood and are part of our natural defense to infection, can prevent new HIV infections.
The first trial, called HVTN 702, relies on the classical approach of active immunization. Here a vaccine designed to mimic an infection causes the body to make antibodies to HIV.
The second trial, called AMP or antibody-mediated protection, will run in parallel to the first trial. It will use manufactured antibodies that are infused into the body. This approach, called passive immunization, has been employed for over a 100 years to treat a variety of infectious diseases. This has only recently become an option for HIV. This trial is unprecedented in HIV prevention research.
We are at a pivotal stage in HIV vaccine development. Conducting two large scale efficacy trials in the region of the world with the highest HIV prevalence heralds a new more aggressive approach to tackle what is our most serious public health threat.
Active Vaccination
The HVTN 702 vaccine trial was inspired by the results of an earlier trial—RV144—conducted in Thailand. This trial showed a modest 31 percent efficacy and provided the first ever indication that a vaccine against HIV may be possible.
This vaccine is now being tested in southern Africa, but it has been tailored to match the viruses circulating in this region. There are also other modifications that are intended to improve on the efficacy of the vaccine which will hopefully facilitate its licensure.
The vaccine comprises two components that stimulate the body’s disease fighting immune helper cells as well as antibodies.
The first, a cellular response, uses a harmless canarypox virus that has been engineered to carry small pieces of HIV. This tricks the body into thinking it is under attack so that it mounts an immune response to HIV.
For the other component—the antibody response—soluble protein derived from the outer envelope coat of the virus are recreated in the laboratory, and used to elicit antibodies to HIV. In RV144, individuals who developed antibodies to a small fragment of envelope called the variable region 1 and 2 (V1V2) had a reduced risk of HIV infection. As such, these immune responses are used to benchmark future trials.