Tenderness at acupuncture point SP6 (Sanyinjiao) is linked to incidences of menstrual cramping with pain. Tenderness at this lower leg acupuncture point has been associated with dysmenorrhea in Traditional Chinese Medicine (TCM) for over a thousand years. Now, researchers have completed a randomized study to test the scientific basis for this phenomenon. The researchers discovered a significant “tenderness at Sanyinjiao (SP6) exists in women undergoing primary dysmenorrhea.”
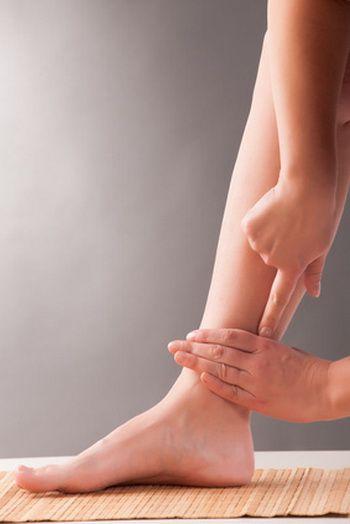
Acupuncture point SP6 (Sanyinjiao) Shuttersock





