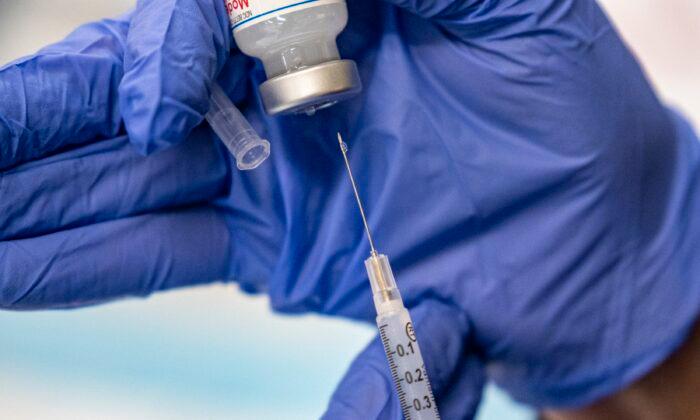
A U.S. health agency on April 7 announced the launch of a study of allergic reactions to two COVID-19 vaccines.
A systemic allergic reaction to a vaccine means a reaction occurs in one or more parts of the body beyond the site of the injection.
If such reactions occur during the study, investigators will assess whether they’re more frequent in participants with a history of reactions or disorder versus other trial participants. Investigators will also probe the biological mechanism behind the reactions and try to pinpoint whether genetic patterns or other factors could predict which people are most at risk.
The trial is being funded and sponsored by the National Institute of Allergy and Infectious Diseases (NIAID), which is part of the National Institutes of Health.
“The information gathered during this trial will help doctors advise people who are highly allergic or have a mast cell disorder about the risks and benefits of receiving these two vaccines. However, for most people, the benefits of COVID-19 vaccination far outweigh the risks.”
The trial will enroll 3,400 adults between the ages of 18 and 69 at 35 allergy-research centers across the nation. About 6 in 10 of the participants must have either a history of severe allergic reactions or a diagnosis of a mast cell disorder. The others must not.
Approximately two-thirds of volunteers will be female, since the vast majority of cases of anaphylaxis to COVID-19 vaccines have occurred among women.
Participants will be randomly assigned to receive a vaccine or a placebo followed by a vaccine. Every participant will ultimately get two doses of a vaccine.
Results are expected in late summer.

The agency didn’t immediately respond to an inquiry asking why it’s taken so long to launch a trial exploring allergic reactions to vaccines. Fauci and other health officials weren’t asked about and didn’t mention the trial during a virtual press briefing on April 7.
Both Moderna and Pfizer received emergency use approval for the COVID-19 shots in December 2020.
More than 168 million doses have been administered in the United States as of April 6. All but 4.3 million are from Moderna or Pfizer.
According to U.S. officials, the allergic reaction rate post-vaccination has since dropped to approximately two to five cases per million. The Centers for Disease Control and Prevention (CDC) and Food and Drug Administration describe anaphylaxis as “rare” following a COVID-19 shot.
In a small percentage of cases, the patient has died.
Health officials say that a review of available clinical information including death certificates, autopsy, and medical records revealed no evidence that vaccination contributed to the patient deaths.
Facilities administering COVID-19 vaccines should have at least three doses of epinephrine available at all times and should observe people getting vaccinated for at least 15 minutes, according to the CDC. Those with a history of allergic reactions to vaccines or a history of anaphylaxis due to any cause should be observed for at least 30 minutes.
Signs of severe allergic reactions include throat tightness, nausea, dizziness, agitation, and a sudden increase in secretions from the eyes, nose, or mouth.
Symptoms of anaphylaxis often occur within 15 to 30 minutes of vaccination, though it can sometimes take several hours for symptoms to appear.