Investing in skin cancer prevention in Australia could both save lives and significantly reduce the nation’s $2 billion (approx US$1.45 billion) a year in treatment costs, experts say.
Led by Associate Professor Louisa Gordon of the QIMR Berghofer Medical Research Institute, the paper points out that while new systemic treatments for melanoma cost the Australian Government about $500 million (approx US$362 million) in 2020-21, the cost of treating the much more common, but less lethal keratinocyte cancers is far higher, reaching $1.3 billion (approx US$940 million) in 2018-2019.
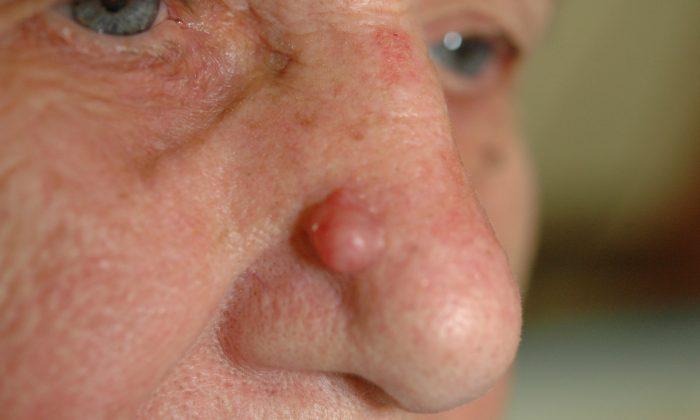
Keratinocyte skin cancers, on the other hand, refer to basal cell and squamous cell carcinomas, which account for around 80 percent and 20 percent of skin cancers respectively. These cancers grow more slowly and are far less likely to spread to other parts of the body.
Overall, skin cancers cost the Australian health economy approximately $2 billion annually, but there has been no investment in skin cancer prevention at a national level for over a decade.
The paper includes findings from two Australian studies, which show that prevention interventions are highly cost-effective, with every dollar spent on skin cancer prevention bringing an investment return two to four times greater.
“What our paper shows is that while skin cancer is a major burden on our health system, prevention does work,” Associate Professor Gordon said.
One of the study’s authors also found that in the general population, consistent sun protection was more successful at reducing skin cancers than early detection through mass screening.
“It’s a really important reminder to put on your hat and sunscreen when you hit the beach this summer. And it’s not just melanoma we need to be worried about—far more common skin cancers can harm our health and also add to the financial strain on our health system,” Gordon said.
The paper’s authors are pushing for studies into cost-effectiveness in order to assess the relative benefits of preventative measures such as workplace shade, personal protective wear and school-based protective clothing.
Another means of increasing sun protection could be government regulation to reduce the price of approved sunscreen products.
The authors note that currently, the average sunscreen use per Australian per year is just 33 teaspoons, 0r less than a teaspoon a week, a tiny amount considering that one teaspoon of sunscreen will only protect one limb for two hours.
“Investment in preventing skin cancers using public health approaches is the hallmark of cost-effective healthcare with evidence consistently showing cost benefits to government and society,” the authors conclude.