NEW YORK—Thirteen more people were diagnosed with Legionnaires’ disease in the Morris Park section of the Bronx. Although one patient has died, medical specialists are saying that the diagnoses itself should be seen as a good thing.
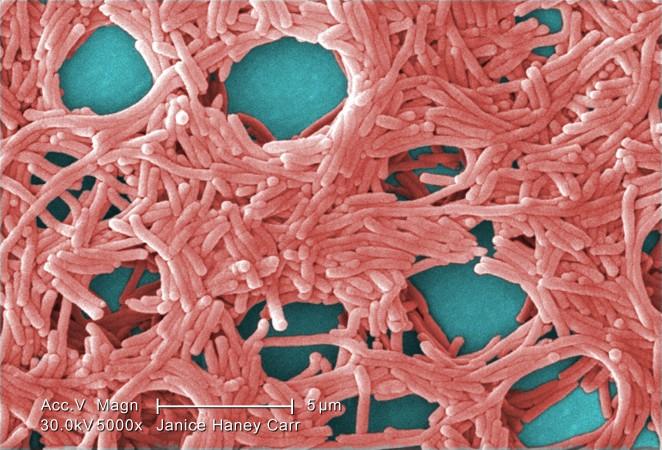
“It’s not an outbreak. It’s an outbreak of diagnosis,” said Janet Stout, a microbiologist who has researched Legionella, the bacteria that causes Legionnaires’ disease, for more than 30 years.
Legionnaires’ disease, a rare but severe form of pneumonia, had taken 12 lives and sickened more than 120 people in July and August during an unrelated outbreak in South Bronx.
But the increase of Legionnaires’ infections doesn’t necessarily indicate that more people are getting sick. It means more doctors are testing for it, showing a critical shift in the New York medical establishment’s attitude toward the disease that can potentially save many lives.
Legionella is a bacteria that is commonly found in the water supplies of large buildings. It doesn’t pose any danger to most healthy people. But it can be life-threatening for the elderly and people with weak immune systems. Since it is an uncommon illness, Legionnaires’ disease has historically been misdiagnosed as some other form of pneumonia.