Hospitals in New York can use one ventilator to treat two COVID-19 patients, Gov. Andrew Cuomo announced on Thursday.
The state projects a need for 30,000 ventilators and only has 15,000 on hand, officials said earlier in the week.
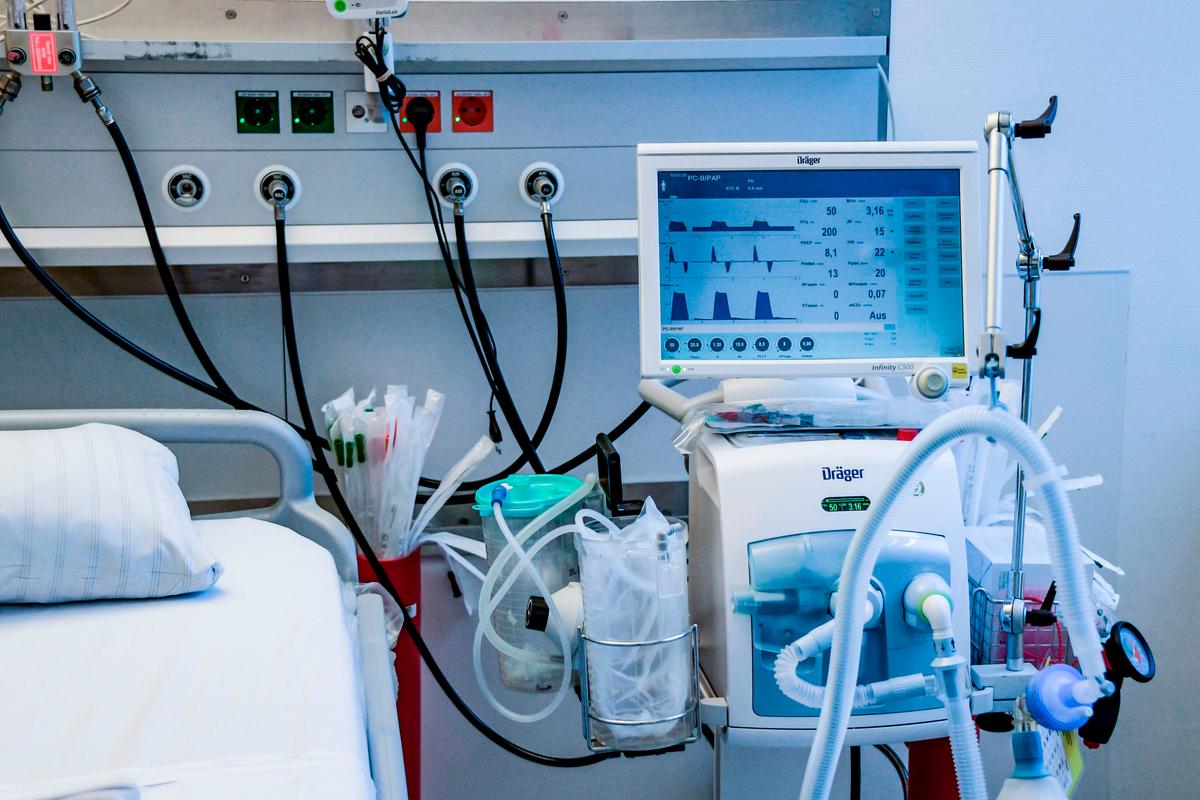

Hospitals in New York can use one ventilator to treat two COVID-19 patients, Gov. Andrew Cuomo announced on Thursday.
The state projects a need for 30,000 ventilators and only has 15,000 on hand, officials said earlier in the week.