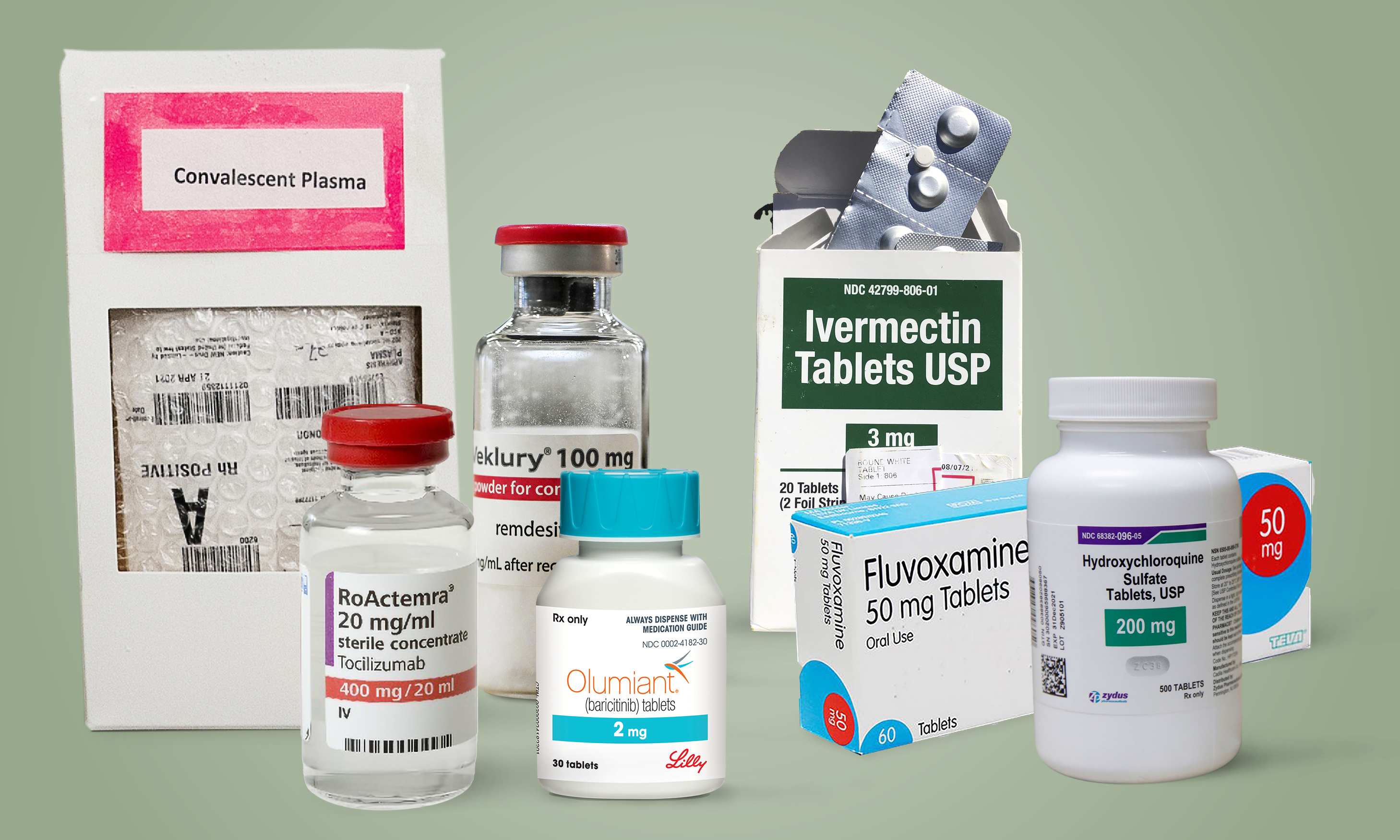
A variety of approved and non-FDA approved COVID-19 treatments. Illustration by The Epoch Times
A variety of approved and non-FDA approved COVID-19 treatments. Illustration by The Epoch Times
This copy is for your personal, non-commercial use only. Distribution and use of this material are governed by our Subscriber Agreement and by copyright law. For non-personal use or to order multiple copies, please contact The Epoch Times Reprints.
