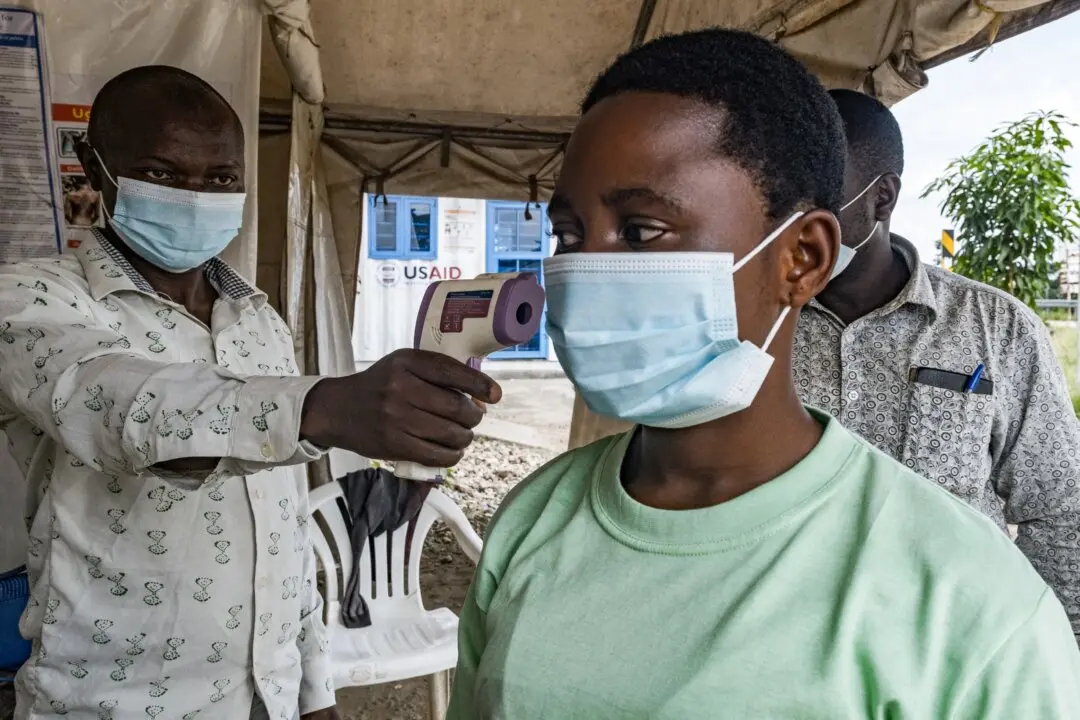
COVID-19 metrics in southern states such as Florida have plummeted in recent weeks while rising in many northern states, including heavily vaccinated states.
Confirmed COVID-19 cases in Mississippi have plunged some 95 percent to 268 on Oct. 7 from the peak of 5,018 on Aug. 19. COVID-19 related hospitalizations in the state, one of the worst-hit in the nation, dropped to 403 on Oct. 7 from 1,667 on Aug. 19.