One of Australia’s leading medical research institutes specialising in COVID-19 has said the country still has a long way to go before achieving herd immunity.
Although the federal government’s roadmap out of lockdown did not mention herd immunity, it also pointed to the possibility that the country will not open its borders until two-thirds of the population are vaccinated.
Herd immunity, also known as “population immunity,” occurs when a large portion of a community becomes immune to a disease, either through infection or vaccination, making the virus not spread easily.
According to the World Health Organisation, scientists around the world are “still working to find and develop treatments for COVID-19,” with research being carried out on Ivermectin—which costs under $10 a tablet—and other drugs that are currently yet to be recommended by the United Nations body for use despite showing promise for use as prophylactics. Meanwhile, Remdesivir, which costs over $4,000 for five days of treatment, has been approved for use as a COVID-19 treatment in the United States.
The Burnet Institute recommended that public health measures such as QR check-ins, social distancing, and wearing masks remain necessary even with high vaccination rates as it is not yet clear the extent to which the emergency use vaccines have been able to prevent transmission.
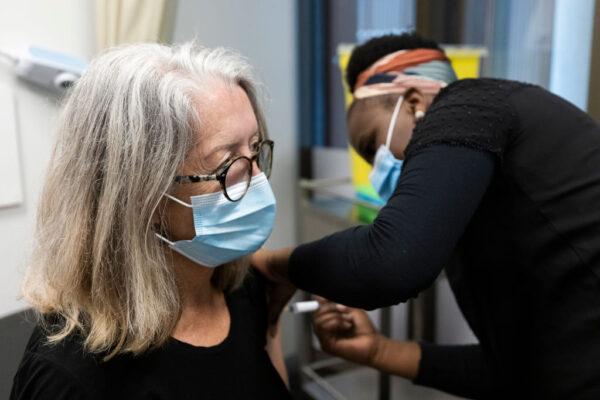
Dr. Dicky Budiman, an epidemiologist at Griffith University’s Center for Environment and Population Health, told The Epoch Times that Australia has a “long journey” to go before reaching the vaccination threshold.
“Let’s say after we achieve the threshold of 80 percent or 90 percent of the total population fully vaccinated; then we still need to see if the vaccines are protecting people from transmission,” Budiman said.
“This is something we still need to see in the real world because without vaccine efficacy, there’s no such thing of herd immunity.”
He estimated it would take around two years to achieve herd immunity and one year to reach the “optimal vaccination rate,” which is “about 200 to 500 vaccine doses per day.”
The epidemiologist also noted that getting the vaccines alone will not secure a ticket back to normal life, although it can provide more protection.
“Of course, the vaccines themselves do not 100 percent guarantee that you will not be infected and that you won’t transmit COVID-19 to others when you got infected,” he said.
“It means we need public health measures because vaccination is not the sole strategy.”
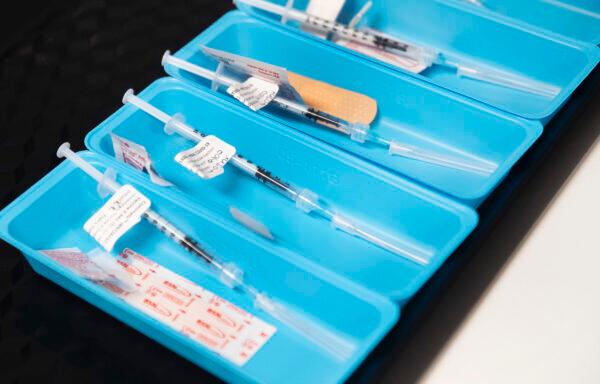
However, scientists are questioning whether achieving the herd immunity threshold can spell the end of the virus, considering the complexities and challenges of the pandemic.
The journal noted that factors such as the spread of new variants, limited efficacy and side effects of the vaccines, lack of data on how long the immunity can last, uneven speed and distribution of vaccine rollout, are believed to be challenging the idea of achievable herd immunity.
Australia’s confidence in the vaccine has also been dropping due to concerns over the vaccines’ side effects, such as the rare blood clotting linked to the AstraZeneca vaccine and heart inflammation linked to the Pfizer and Moderna shots.





Friends Read Free